Transient synovitis
Definition
Transient synovitis of unknown etiology with complete resolution
Epidemiology
Most common cause of hip pain
- age 3 - 10 age
- peak 6 years of age
- more common boys
Etiology
Infectious - associated with viral URTi
Trauma - history of injury
Clinical
Acute onset of unilateral hip pain
Limp
Hip held in flexion and external rotation
Restricted ROM
May be low-grade fever < 38°
Differential diagnosis
Septic Arthritis
Osteomyelitis
Perthes / SCFE
Juvenile rheumatoid arthritis
Lyme arthritis - serology
Kocher Criteria for Septic arthritis
- 4 criteria for risk of septic arthritis
- ESR > 40
- WCC > 12,000
- fever >38.5
- inability to weight-bear
- Risk: 0/4 (.2%) 1/4 (3%), 2/4 (40%), 3/4 (93%), 4/4 (99%)
Caird criteria
- Kocher criteria + CRP > 2
- all 5 positive: septic arthritis 98%
- 311 children with acute hip pain and effusion on ultrasound
- 9% culture proven septic arthritis
- non weight bearing and CRP > 20 strongest predictors
False negatives
Kingella kingae
- child < 4
- can have normal blood parameters
- need hip aspiration and blood culture
- 34 culture proven cases of Kingella hip septic arthritis
- Kocher criteria diagnosis < 40%
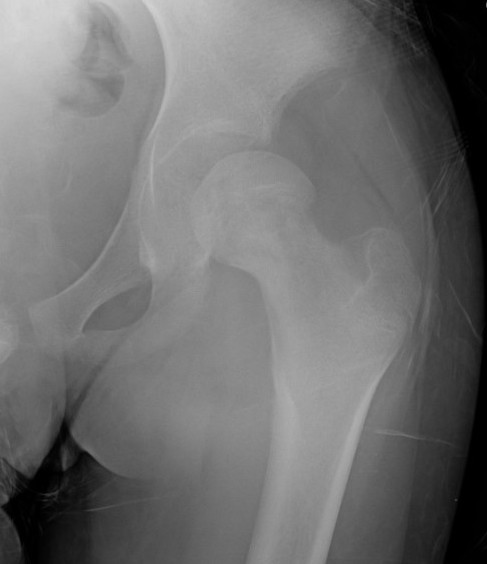
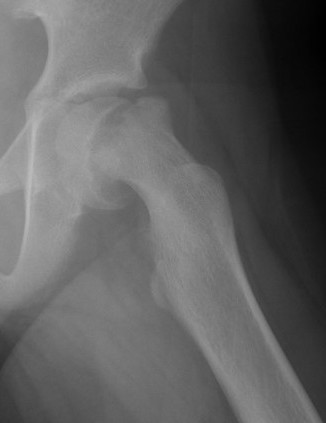
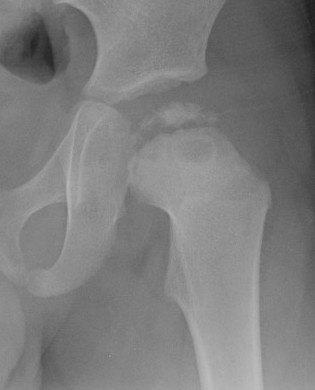
Xray
Normal with transient synovitis
Hip subluxation with septic arthritis

SCFE / Perthes
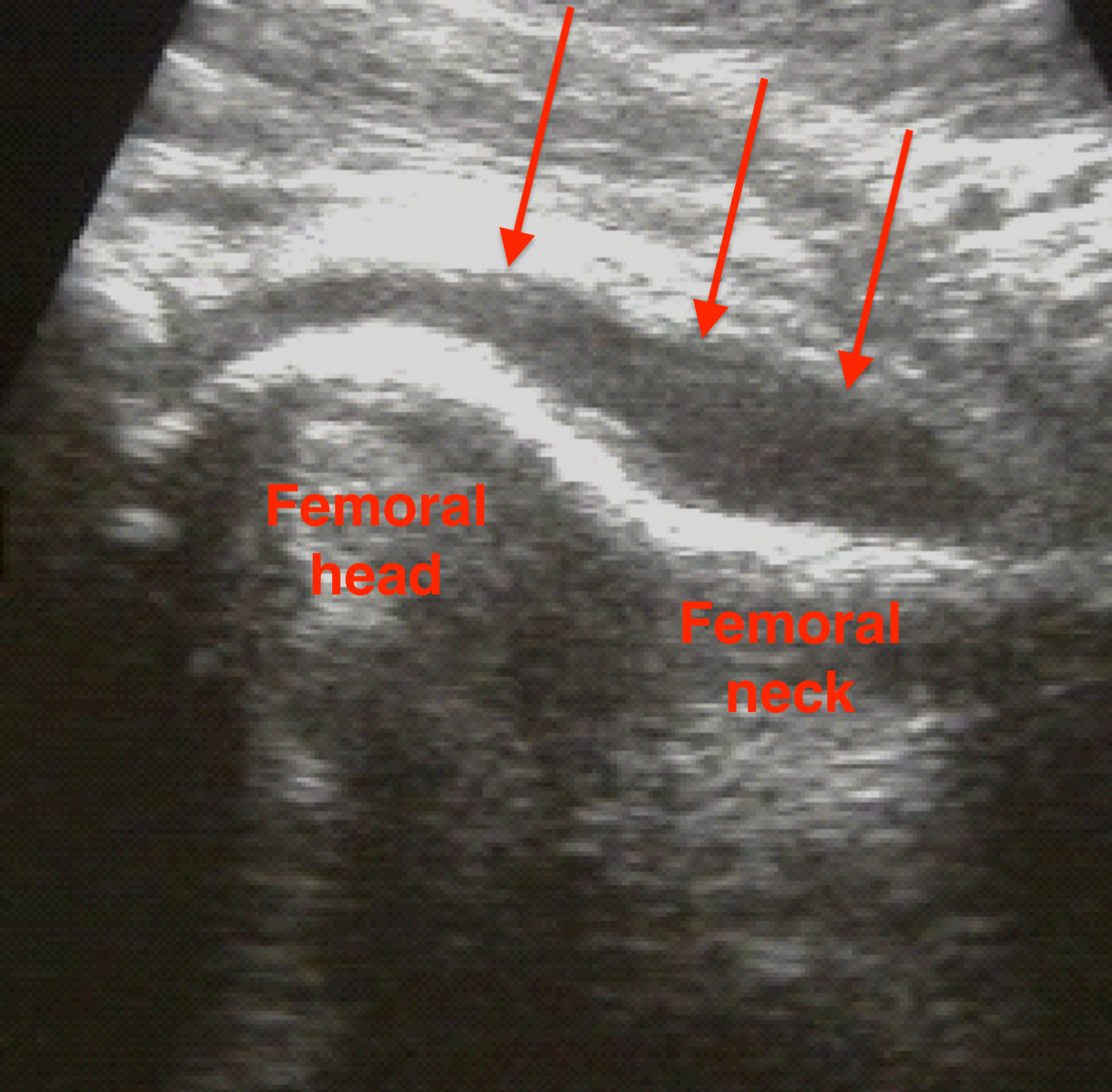
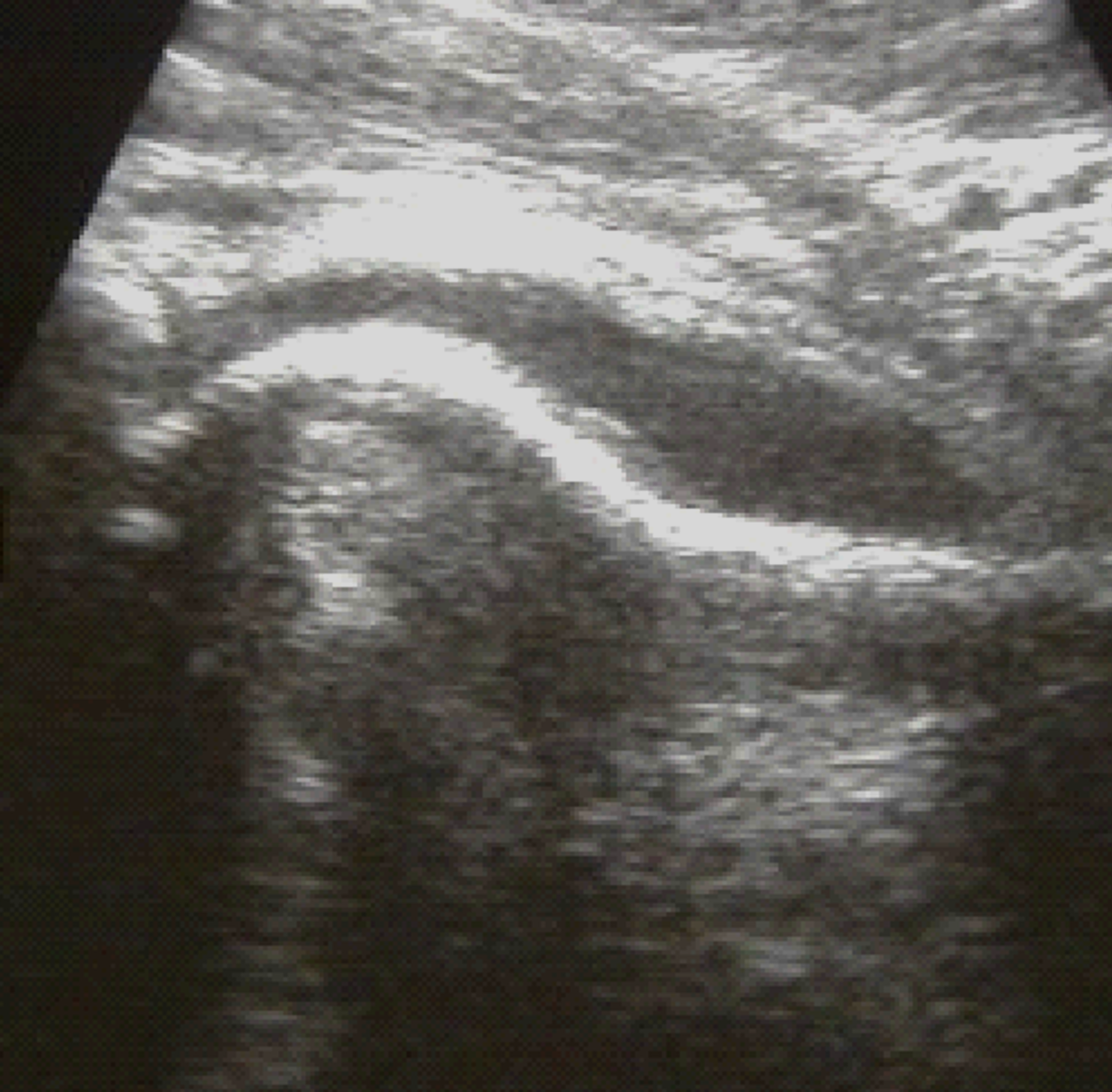
Ultrasound
Effusion

Joint aspiration
Findings
- WBC >50,000 cells / uL
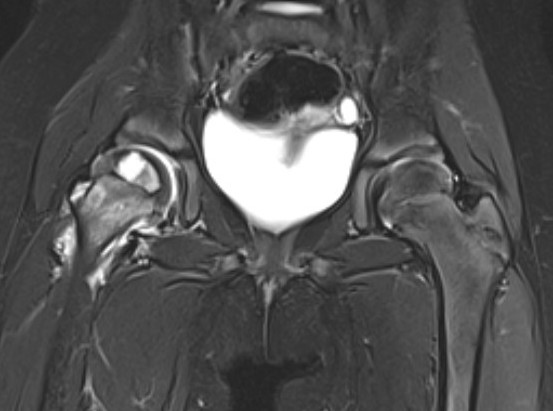
MRI
Adam et al Eur J Radiol Open 2022
- meta-analysis of MRI distinguishing between transient and septic arthitis
- bone marrow changes - 99% specific for septic arthritis
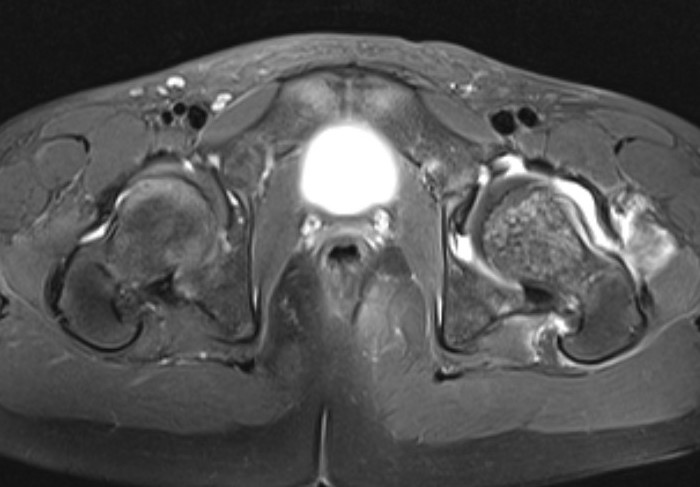
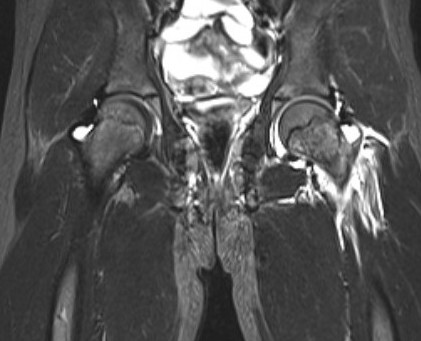
Fluid in hip joint
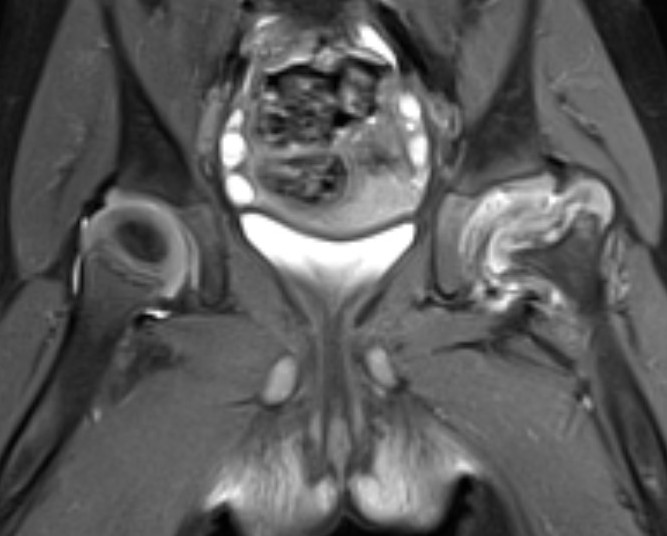
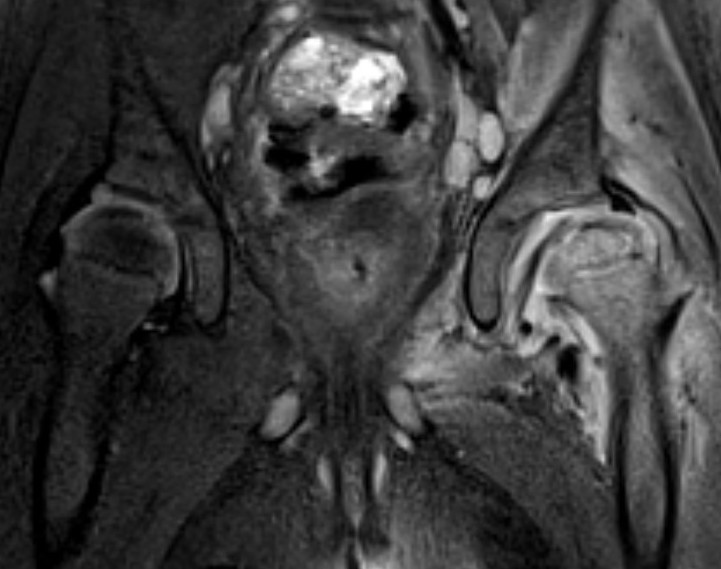
Subluxation of the hip joint with effusion and bone marrow changes
Proximal femoral osteomyelitis

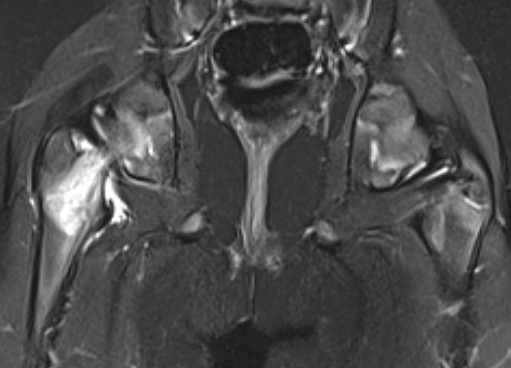
Bone marrow edema and osteomyelitis in the femoral head
Management transient synovitis
Options
Rest
NSAIDS
Symptoms generally improve after 24 - 48 hours
Symptoms generally resolve in 1 - 2 weeks
Recurrence
- can occur
- may be Perthes
Perthes
Xinling et al J Orthop Surg Res 2024
- systematic review of incidence of Perthes after transient synovitis hip
- overall incidence Perthes 2.7%
- recurrent transient synovitis Perthes 36%
Management Septic arthritis
Bacteria
Staph aureus most common
- MRSA increasingly common
- Group B Streptococcus
- Kingella Kingae (fastidious organism; increasingly common in < 4 years)
- Gonococcus (Sexually active adolescents)
Options
Arthrocentesis - hip aspiration and lavage
Hip arthroscopy
Arthrotomy and washout
Results
- systematic review of good clinical outcomes of treatments in septic arthritis
- arthrocentesis: 98%
- arthroscopy: 95%
- arthrotomy: 90%
- systematic review of repeat surgery after treatment in hip septic arthritis
- arthrocentesis: 15%
- arthroscopy: 14%
- arthrotomy: 3%
- inferior long term outcomes with arthrotomy
Hip arthrotomy technique
AO foundation Smith Peterson approach to pediatric hip PDF
POSNA open hip arthrotomy for septic arthritis video
No antibiotics unless positive blood culture
Smith Peterson approach
- bikini incision over AIIS
- interval between sartorius and TFL
- interval between rectus femoris and gluteus medius
- capsulotomy
Drill proximal femoral metaphysis / femoral neck
- diagnose / decompress osteomyelitis
Ensure hip is stable
- may require posteroperative spica if unstable
Hip arthroscopy technique
Arthroscopy technique tractionless pediatric hip arthroscopy for septic arthritis
Antibiotics
Broad spectrum initially
Targeted antibiotics with positive culture
Complications
AVN
Chondrolysis
Physeal arrest
Subluxation / dislocation
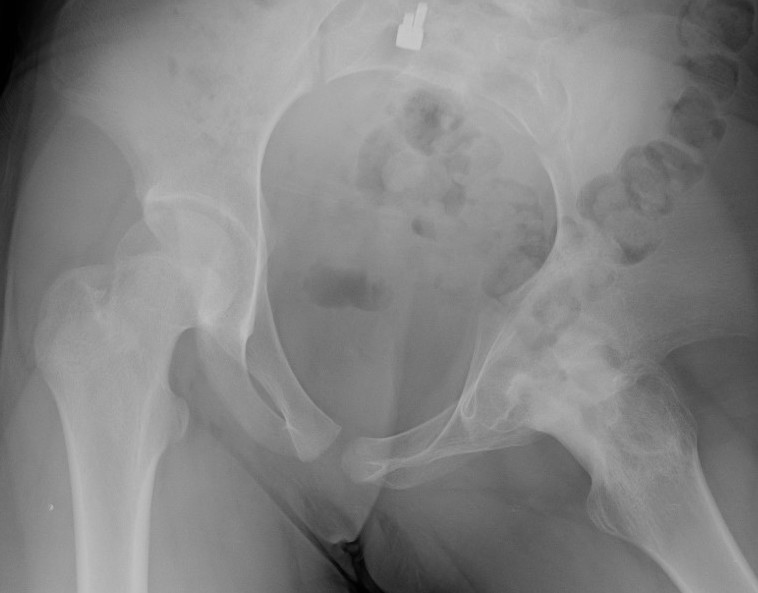
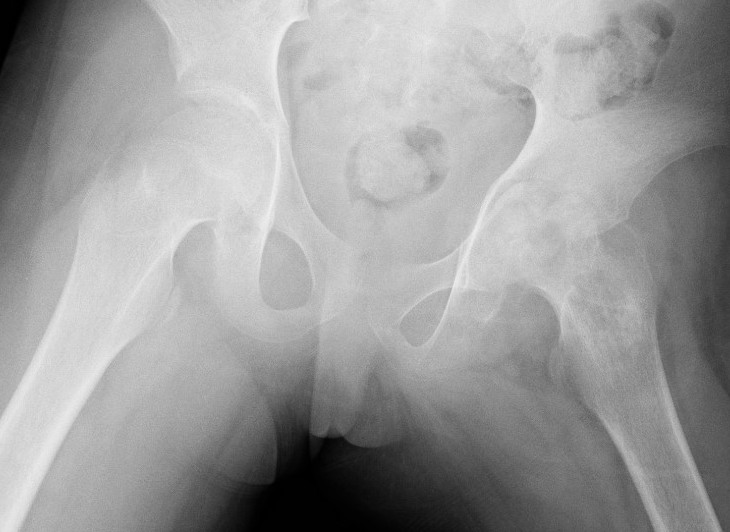
Advanced AVN and collapse after hip septic arthritis
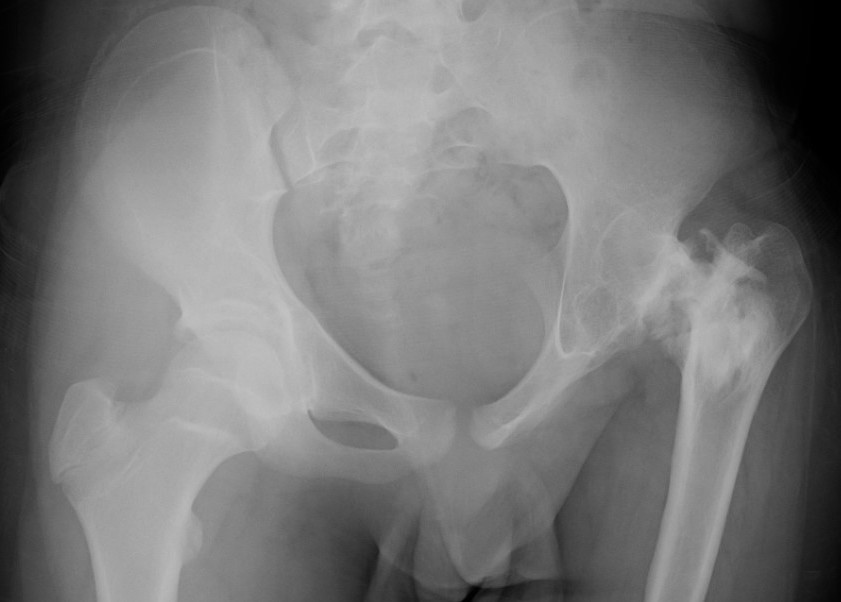
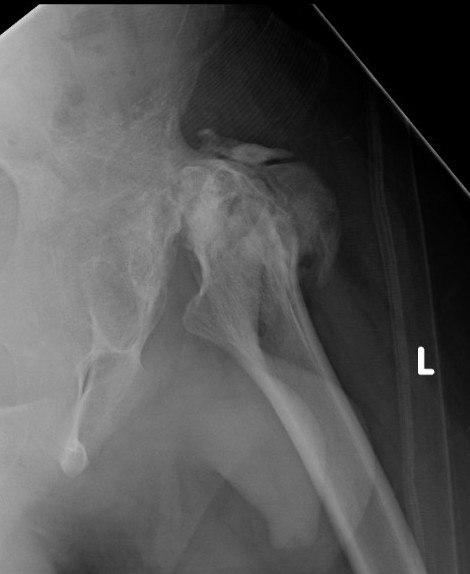
Advanced AVN and collapse after hip septic arthritis
