General Principles
All possible length should be preserved consistent with clinical judgement
- function of amputated stumps decrease progressively with each higher level of amputation
- prosthetic rejection by patient increases with the more proximal amputations
- most ADL'S can be performed adequately with one limb, so don't use prosthesis
- all nerves are drawn distally into wound & sectioned so they retract well proximally to bone level of amputation
Transcarpal
Concept
- can preserve flexion / extension of radiocarpal joint which transmitted partly to prosthesis
Technique
- fashion long palmar, short dorsal flaps in ratio (2:1)
- divide tendons under tension
- divide nerves well proximal to amputation
- divide vessels just proximal to amputation bony level
- divide bones and smooth / round edges
- anchor wrist flexor and extensor tendons to remaining carpal bones in line of pull to allow wrist flexion/extension
Wrist disarticulation
Technique
- fashion long palmar, short dorsal flaps (2:1)
- skin apices 1cm distal to ulnar and radial styloids
- divide vessels, nerves, tendons and open radiocarpal joint
- resect radial / ulnar styloid processes & smoothen bony processes to form a smooth rounded contour
- protect distal radioulnar joint including triangular ligament to preserve supination/ pronation
- insert suction drain and skin closure
Forearm
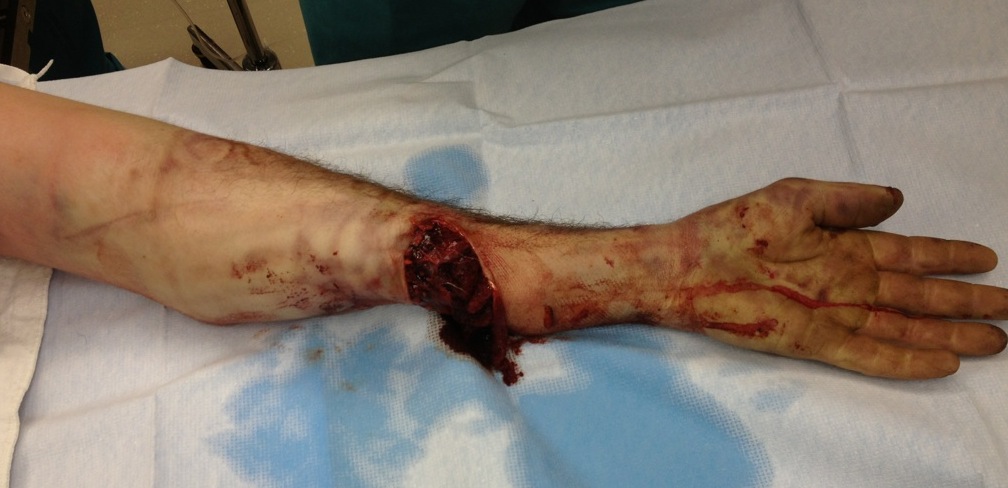
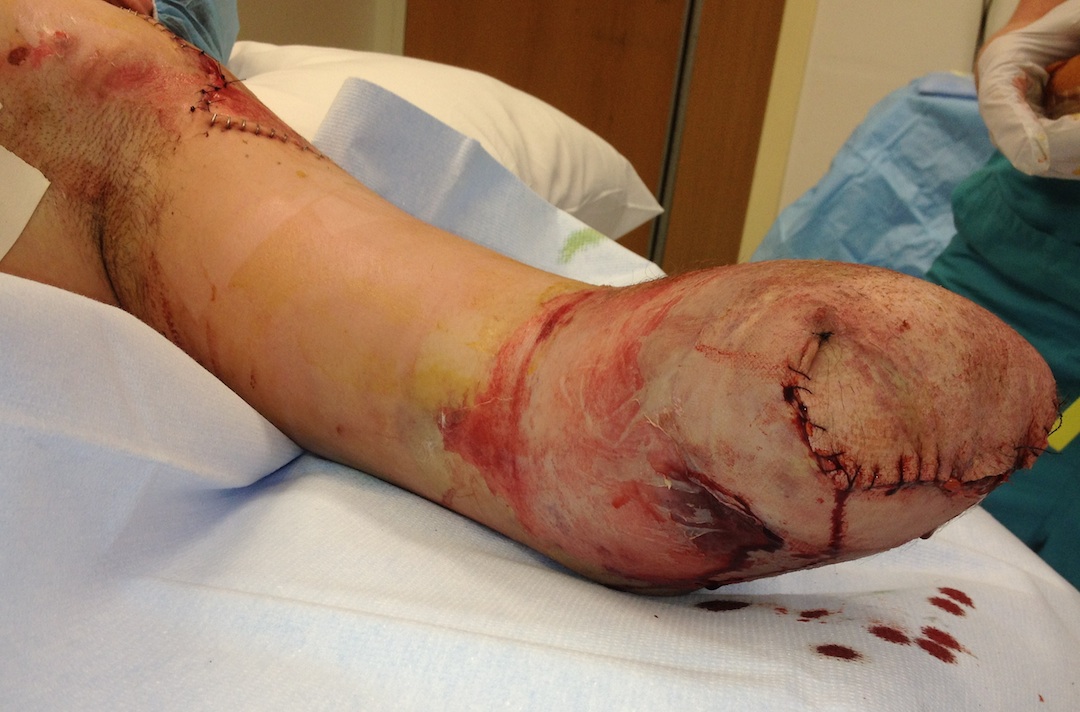
Concept
- preserve as much length as possible (forearm rotation and strength proportional to length retained)
- if circulation compromised, amputation through distal 1/3 forearm are less likely to heal
- distally skin is thin and subcutaneous tissue scant
- junction mid and distal thirds good compromise for amputation level
- short 'below elbow stump' (up to 3.8-5cm long) preferable to through or above elbow
- important to preserve elbow joint
Distal
- skin incision apices at level of bone cut
- ligate radial / ulnar arteries and divide nerves under tension then transverse bone cuts and rasp edges
- fashion FDS flap long enough to be carried around bone ends
- section rest of muscles at level of bone
- suture FDS flap over dorsal fascia
Proximal third
- fashion equal volar and dorsal flaps ideally
- divide muscle bellies distal to bone cuts to allow for retraction
- transverse bone cuts and rasp edges
- if stump is proximal to bicipital radial tuberosity, then resect distal 2.5cm of biceps tendon
- this lengthens stump functionally and enhances prosthetic fitting
- leaves brachialis as principle elbow flexor
Krukenburg's Amputation
- performed as a secondary procedure in 'below elbow' amputation
- converts forearm amputation into radial and ulnar pincers
- need at least 10 cm from olecranon tip & elbow flexion contracture <70o
- classically used in blind bilateral below elbow amputee
Elbow disarticulation
Concept
- good level for amputation due to easy fitting of prosthesis to distal humeral flare
- allows transmission of humeral rotation to the prosthesis (preferable to a more proximal humeral amputation)
- due to modern prosthesis techniques, disarticulation is preferred to proximal humeral amputation
Technique
- equal anterior and posterior flaps with apices at level of humeral epicondyles
- posterior flap extents 2.5cm. distal to olecranon tip
- anterior flap extends just distal to biceps tendon insertion
- divide lacertus fibrosis
- reflect distally flexor origin off medial epicondyle
- expose neurovascular bundle on medial side of biceps tendon
- divide brachial artery, median and ulnar nerves proximal to elbow joint
- free the insertions of biceps and brachialis from radius / ulna
- divide radial nerve as lies between brachialis and BR
- divide transversely extensor mass 6 cm distal to joint line
- divide posterior fascia and triceps tendon near tip of olecranon
- divide anterior joint capsule to complete the disarticulation & remove the forearm
- leave intact articular cartilage of humerus
- suture triceps tendon anteriorly to biceps and brachialis
- suture extensor muscle mass medially to flexor origin muscle stump
Can add distal humeral osteotomy
- create anterior angulation 45o
- aids prosthesis fitting / reduces need for shoulder harness
Above Elbow
Concepts
- most important to preserve limb length
Above elbow prosthesis
- elbow-lock mechanism stabilises joint in full extension, flexion or in a position between
- lock mechanism extends 3.8 cm distally from the end of the prosthetic socket
- therefore most distal bone section should be 3.8cm from end of humerus to allow room for this mechanism
Supracondylar level
- equal anterior and posterior flaps at length 1/2 diameter of arm at that level
- artery and nerve divided proximal to level of resection
- divide anterior compartment muscle flaps 1.3cm distal to bone section level so they retract to this level
- free triceps insertion off olecranon & preserve as a long flap
- transverse bone cut 3.8 cm proximal to humerus end and rasp edges
- suture long flap of triceps anteriorly to the fascia over anterior muscles
Proximal to supracondylar level
- equal anterior and posterior flaps
- divide anterior compartment muscles 1cm distal to bone cut to allow retraction
- divide triceps 3.8-5cm distal to bone cut
- suture triceps anteriorly over bone end to anterior muscle fascia
Shoulder amputations
Concept
- shoulder amputation levels require fitting as if for joint disarticulation
- Prosthetic function is severely impaired at shoulder level
- prostheses are used primarily as a holding device when performing activities with both hands
Through surgical neck
Position
- patient supine with sandbag beneath shoulder (patient's back 45 degrees to table)
Anterior incision
- incision from coracoid process, along anterior deltoid border to its insertion
Posterior incision
- along posterior deltoid border to posterior axillary fold
- connect the two limbs of incision by a second incision that passes through axilla then incise anteriorly through axilla
Superficial dissection
- ligate cephalic vein, separate deltoid and pectoralis major in deltopectoral groove
- reflect deltoid laterally
- divide pectoralis tendon at its insertion and reflect medially
Expose neurovascular bundle
- develop plane between pectoralis minor and coracobrachialis to expose neurovascular bundle
- divide axillary artery and vein inferior to pectoralis minor
- divide nerves on stretch so they retract proximal to pectoralis minor
Deep dissection
- divide deltoid insertion and reflect deltoid / lateral skin flap superiorly
- divide teres major and latissimus dorsi at bicipital groove
- divide short and long heads of biceps, triceps and coracobrachialis 2 cm distal to bone cut
- section bone at surgical NOH
Closure
- suture long head triceps, both heads biceps and coracobrachialis over end of humerus
- suture pectoralis major tendon to bone end
- bevel deltoid to allow skin closure
Shoulder disarticulation
Position and incision
- as above
Superficial dissection
- ligate cephalic vein
- separate deltoid and pectoralis major
- retract deltoid laterally and divide insertion
- divide pectoralis major tendon at insertion and reflect medially
Neurovascular bundle
- divide conjoint tendon and P minor on coracoid
- expose neurovascular bundle
- ligate axillary artery and vein and thoracoacromial artery
- divide nerves on stretch so they retract proximal to pectoralis minor
Deep dissection
- reflect deltoid insertion superiorly to expose shoulder joint capsule
- divide teres major and latissimus dorsi at insertions
- after internally rotating arm divide posterior rotator muscles at insertion & posterior capsule
- place arm in extreme external rotation & divide subscapularis anterior joint capsule
- divide triceps at infraglenoid tubercle insertion & divide inferior capsule to severe the limb
Closure
- suture all muscles across glenoid to fill the hollow out (deltoid to inferior glenoid)
- may need to trim prominent anterior acromion to produce smoothly rounded contour
- drain deep to deltoid
Forequarter
Concept
- shoulder girdle amputation
- consists of removal entire shoulder girdle / upper limb in interval between scapula and thoracic wall
- indicated for malignant tumour involving upper humerus or shoulder joint
- atypical skin flaps often used, may require axillary skin grafts
Anterior Approach
Incision
Upper limb of incision
- begins at lateral border sternocleidomastoid
- extends laterally along anterior aspect clavicle
- back across AC joint
- over superior aspect shoulder to scapular spine
- inferiorly along vertebral border of scapula to inferior angle
Lower limb
- starts at mid 1/3 clavicle
- runs inferiorly in deltopectoral groove
- runs posteriorly through axilla to join upper limb incision at inferior scapular angle
Superficial Dissection
- subperiosteally dissect out clavicle
- cut at lateral border sternocleidomastoid and through AC joint
- external jugular divided or retracted
Deep Dissection
- release pectoralis major off humerus and pectoralis minor off coracoid to expose neurovascular structures
- ligate subclavian artery and vein, divide brachial plexus under stretch
- release Lat dorsi & remaining soft tissues that bind shoulder girdle to anterior chest wall and allow limb to fall posteriorly and down
- while holding arm across the chest divide posterior rotator cuff
- divide anterior and posterior muscles holding scapula to thoracic wall
- trapezius / omohyoid / L scapulae / rhomboids / serratus anterior
- suture pectoralis major and trapezius over lateral chest wall
- trim flaps and primary suture
Posterior Approach
Position
- lateral decubitus position near edge of operation table
Incisions
Posterior
- make posterior incision first
- begin at medial end of clavicle, extending laterally along clavicle over acromion process to posterior axillary fold
- along axillary border of scapula to a point inferior to scapular angle
- curve incision medially to end 5cm from midline of the back
- same incision as for anterior approach except posterior limb runs along axillary border of scapula
Anterior
- as above
- starts at mid 1/3 clavicle and runs inferiorly just lateral and parallel to deltopectoral groove
- then runs posteriorly through axilla to join posterior axillary incision at lower 1/3 of axillary border of scapula
Superficial Dissection
- elevate full-thickness skin flaps and subcutaneous tissue to medial border of scapula
- trapezius / lat dorsi divided parallel to medial border of scapula
- divide Levator scap / rhomboids / serratus anterior / omohyoid from scapula
- ligate vessels especially transverse Cervical artery and Transverse scapular artery
- free clavicle and divide at medial end with subclavius
- shoulder falls anteriorly
Deep dissection
- subclavian artery & vein / brachial plexus on stretch (divided close to spine)
- divide P major and minor & remove limb
