Management
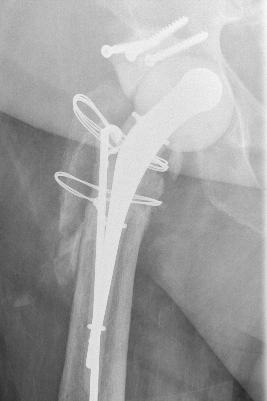
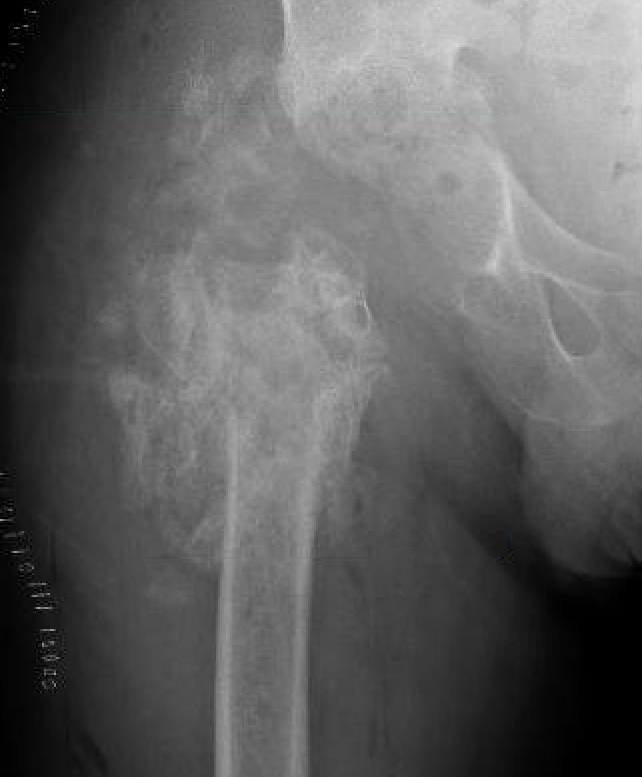
Tsukayama Classification


Patient > 70
Gjertsen et al JBJS Am 2010
- 4335 patients > 70 with displaced subcapital fractures
- minimum 1 year follow up
- 1 year mortality same in each group / 25%
- 22% reoperation in ORIF v 3% in hemiarthroplasty
- more pain / higher dissatisfaction / lower quality life in ORIF group
Hemiarthroplasty
- unipolar monoblock
- unipolar modular
Chronic, non metabolic bone disorder
Characterised by increased bone resorption, bone formation and remodelling
Rare < 40
1 – 3 % population over 60
M > F
Unknown
Paramyxovirus implicated
- measles
- RSV
- canine distemper virus
Electron Microscope
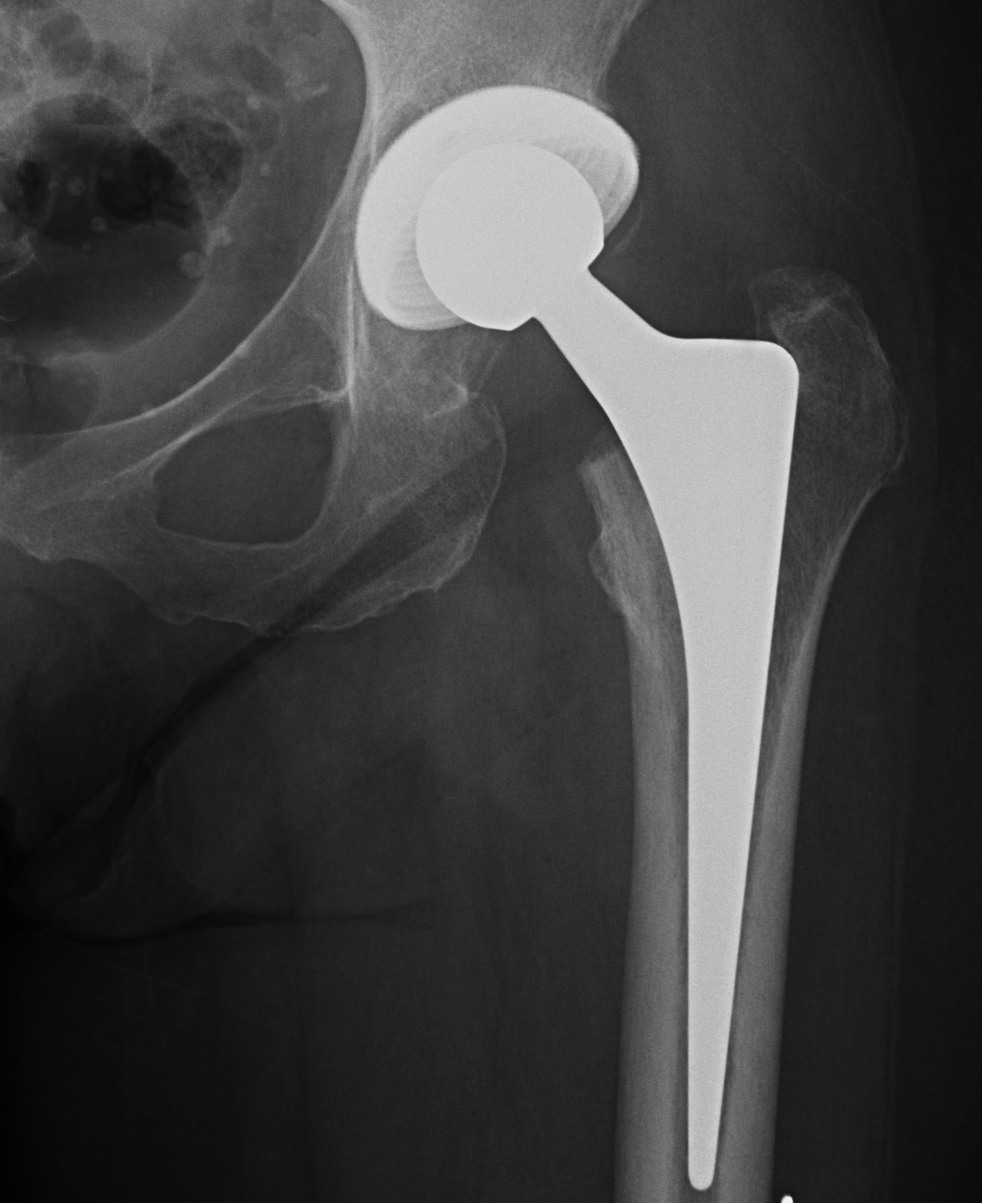
Initial press fit
- implant geometry fits the cortical bone in the proximal femur
- good initial mechanical stability
Biological fixation for success
- good press fit
- minimal micromotion
- bony or fibrous tissue ingrowth or ongrowth
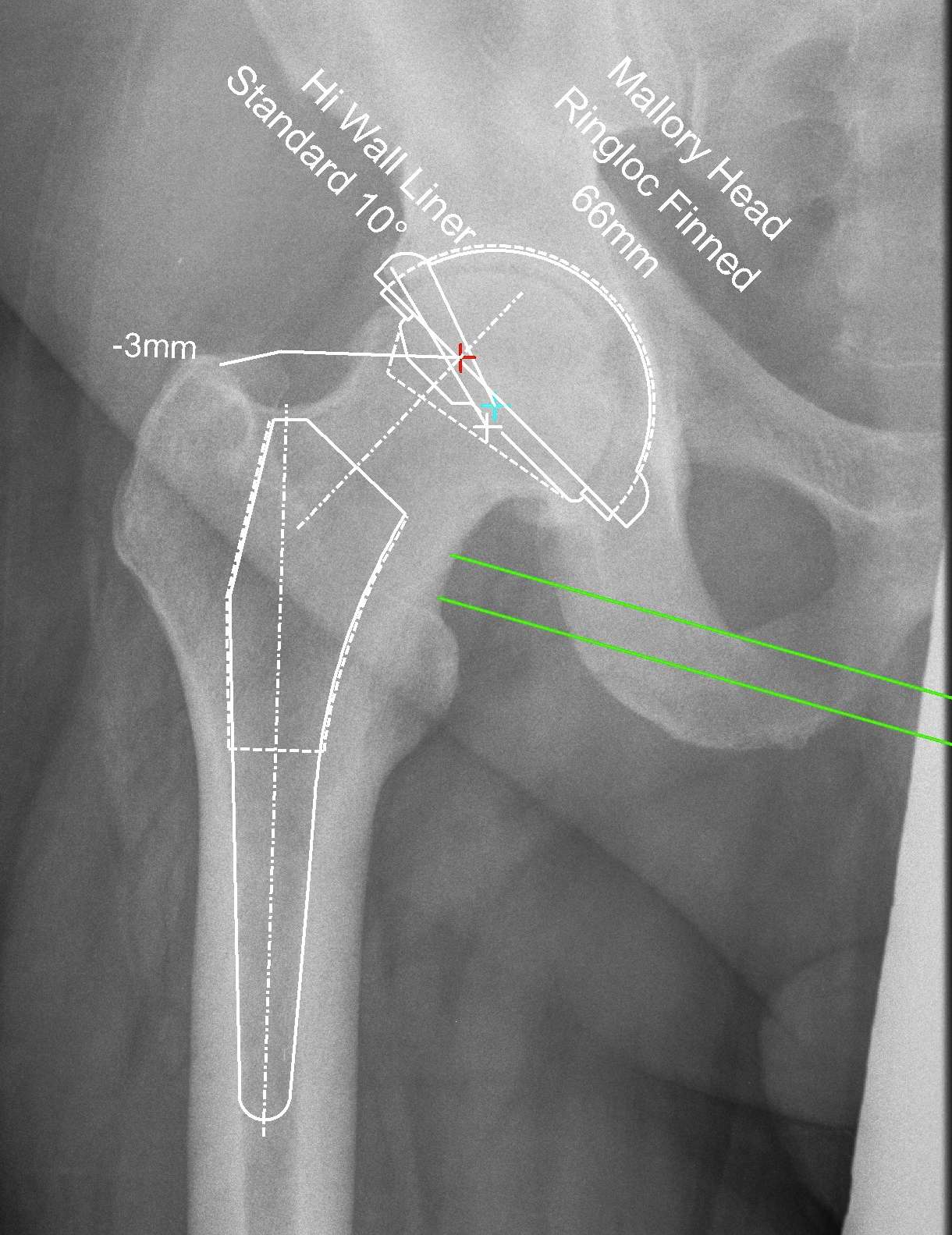
Reproduce the normal anatomical centre of rotation
Restore femoral offset
Maintain equal leg lengths
Usually template off normal hip
1. LLD
2. Offset
3. Femoral component
4. Acetabular component
5. Osteotomy / femoral seating
Peri-operative
- incurred during operation
Post operative
- related to osteolysis / trauma / infection
1994 National Institutes of Health Consensus on THR
Intrinsic
Infection
Loosening
Thigh pain in uncemented
- micro motion at distal end of stem
- modulus mismatch
Stress fracture / insufficiency fracture
- pubic rami, sacral
Intra-operative fracture
Prosthesis failure
Subtle instability
Extrinsic