Multidirectional Instability
Definition
Instability in at least 2 planes
- postero-inferior
- antero-inferior
- antero-postero-inferior
Epidemiology
Recognised as a common problem
- often misdiagnosed
Most patients athletic
Instability in at least 2 planes
- postero-inferior
- antero-inferior
- antero-postero-inferior
Recognised as a common problem
- often misdiagnosed
Most patients athletic
A GH dislocation which has been missed for a significant period of time
- time period is arbitary
- > 3-6 weeks
Humerus soft and osteoporotic
Significant soft tissue contractures
1. Anterior / subcoracoid dislocation
Beware
- scarring to NV structures
- RC tears including SSC, especially > 40
Traumatic initial cause in 95%
M:F 2:1
Age of initial dislocation inversely related to recurrence rate
- patients younger than 20 have a redislocation rate of 90%
- between 20 - 40 years, redislocation rate of 60%
- patients > 40 years have a 10% rate of dislocation but a higher rate of cuff tears (up to 40% in patients > 60yrs)
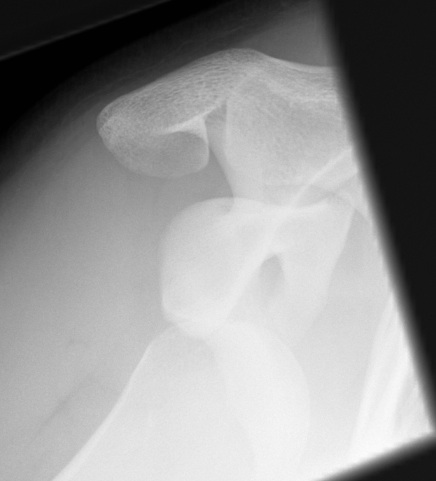
Most common form of shoulder instability
- young males
- M:F = 2:1
Indirect ER and abduction moment on arm
- disruption of anterior stabilisers
Initial injury
- severe pain in shoulder
Idiopathic inflammatory condition
- characterised by progressive shoulder pain & stiffness
- due to contracture of capsuloligamentous structures
- spontaneously resolves
2% incidence
- 40 - 60 years
- Women 2:1
Sedentary workers
- Non-dominant limb
Bilateral in 10 - 40%
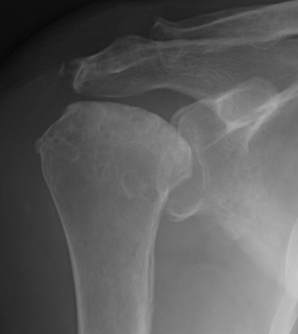
Much less common than hip OA
- usually presents late
Similar causes as hip (AS IT GRIPS 3C)
Alcohol / Steroid / Trauma / Idiopathic
Gauchers
RA / RTx
Sickle Cell
- stabilise patient with beanbag or lateral rests
- apply skin traction to forearm
- place traction pole at foot of table opposite surgeon
- suspend arm with 10 lb weight
- abduction 60°
- forward flexion of 20°
- tilt top shoulder posteriorly 30° so that glenoid is parallel wwith bed
- mark bony landmark
- prep & free drape
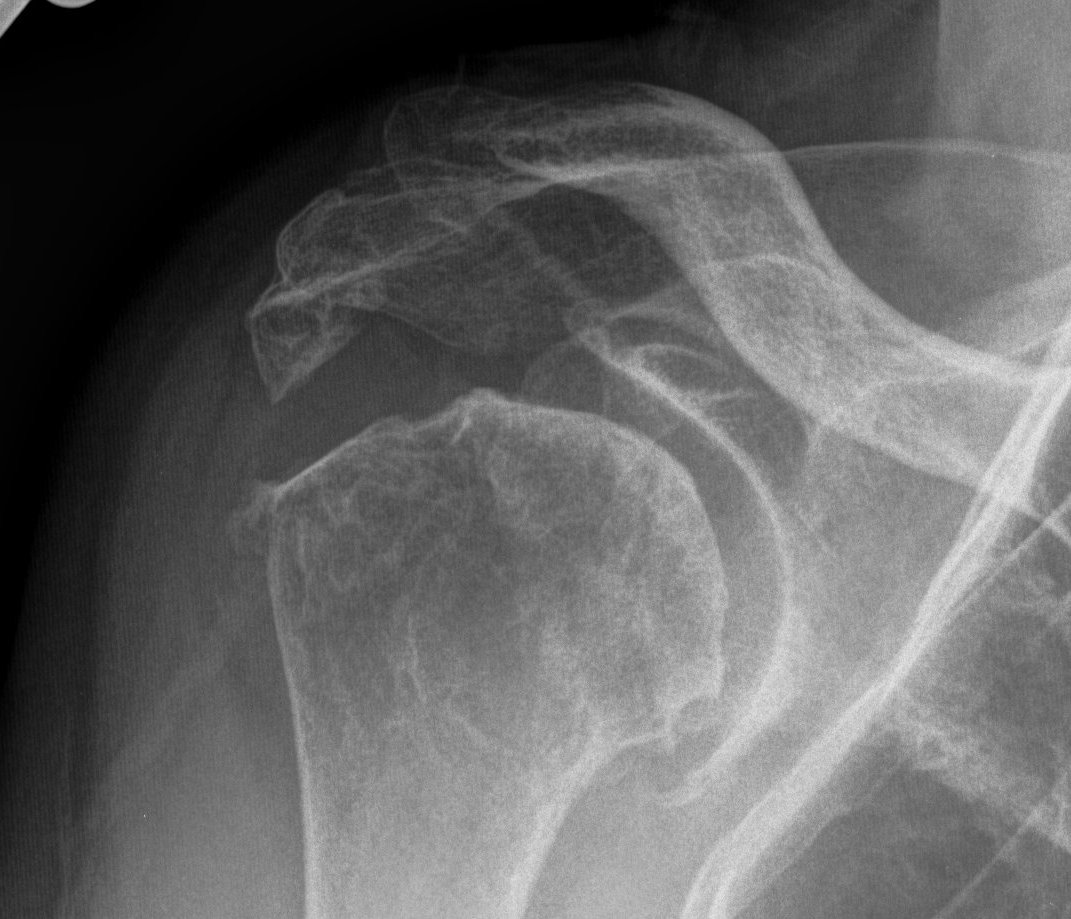
Rotator cuff
- often deficient
Bone stock
- often deficient
Glenoid
- often posterior version
1. TSR
Indications
- cuff intact
Indications have narrowed
- due to success of shoulder arthroplasty
1. Chronic infections of GHJ
2. Stabilization in paralytic disorders
3. Post-traumatic brachial plexus palsy
4. Salvage of failed GHJ Arthroplasty
- may need bone graft procedures
5. Arthritic diseases unsuitable for arthroplasty / young patient
All possible length should be preserved consistent with clinical judgement
- function of amputated stumps decrease progressively with each higher level of amputation
- prosthetic rejection by patient increases with the more proximal amputations
- most ADL'S can be performed adequately with one limb, so don't use prosthesis
- all nerves are drawn distally into wound & sectioned so they retract well proximally to bone level of amputation